Gitelman syndrome is a rare genetic autosomal recessive disorder that affects the sodium-chloride cotransporter in the distal convoluted tubule of the nephron and causes electrolyte abnormalities. The syndrome presents clinically with symptoms of hypokalemia and hypomagnesemia. Diagnosis is based on clinical presentation and laboratory testing (showing hypokalemia, hypomagnesemia, metabolic alkalosis, and hypocalciuria), and confirmed with genetic testing. The mainstay of management is electrolyte supplementation. The prognosis Prognosis A prediction of the probable outcome of a disease based on a individual's condition and the usual course of the disease as seen in similar situations. Non-Hodgkin Lymphomas is good, but hypokalemia Hypokalemia Hypokalemia is defined as plasma potassium (K+) concentration < 3.5 mEq/L. Homeostatic mechanisms maintain plasma concentration between 3.5-5.2 mEq/L despite marked variation in dietary intake. Hypokalemia can be due to renal losses, GI losses, transcellular shifts, or poor dietary intake. Hypokalemia must be monitored to prevent cardiac arrhythmias and potential cardiac arrest Cardiac arrest Cardiac arrest is the sudden, complete cessation of cardiac output with hemodynamic collapse. Patients present as pulseless, unresponsive, and apneic. Rhythms associated with cardiac arrest are ventricular fibrillation/tachycardia, asystole, or pulseless electrical activity. Cardiac Arrest.
Last updated: Oct 31, 2022
Gitelman syndrome (GS) is a rare genetic autosomal recessive Autosomal recessive Autosomal inheritance, both dominant and recessive, refers to the transmission of genes from the 22 autosomal chromosomes. Autosomal recessive diseases are only expressed when 2 copies of the recessive allele are inherited. Autosomal Recessive and Autosomal Dominant Inheritance disorder that affects the thiazide-sensitive Na+–Cl– cotransporter (NCC) in the distal convoluted tubule (DCT), leading to a salt-wasting tubulopathy.
The DCT is the smallest portion of the duct system in a nephron Nephron The functional units of the kidney, consisting of the glomerulus and the attached tubule. Kidneys: Anatomy. It measures about 5 mm MM Multiple myeloma (MM) is a malignant condition of plasma cells (activated B lymphocytes) primarily seen in the elderly. Monoclonal proliferation of plasma cells results in cytokine-driven osteoclastic activity and excessive secretion of IgG antibodies. Multiple Myeloma in size and starts from the macula Macula An oval area in the retina, 3 to 5 mm in diameter, usually located temporal to the posterior pole of the eye and slightly below the level of the optic disk. It is characterized by the presence of a yellow pigment diffusely permeating the inner layers, contains the fovea centralis in its center, and provides the best phototropic visual acuity. It is devoid of retinal blood vessels, except in its periphery, and receives nourishment from the choriocapillaris of the choroid. Eye: Anatomy densa. Characteristics of the DCT are as follows:
Gitelman syndrome leads to the loss of function Loss of Function Inflammation of the NCC → electrolyte abnormalities due to interference with the normal functioning of the DCT
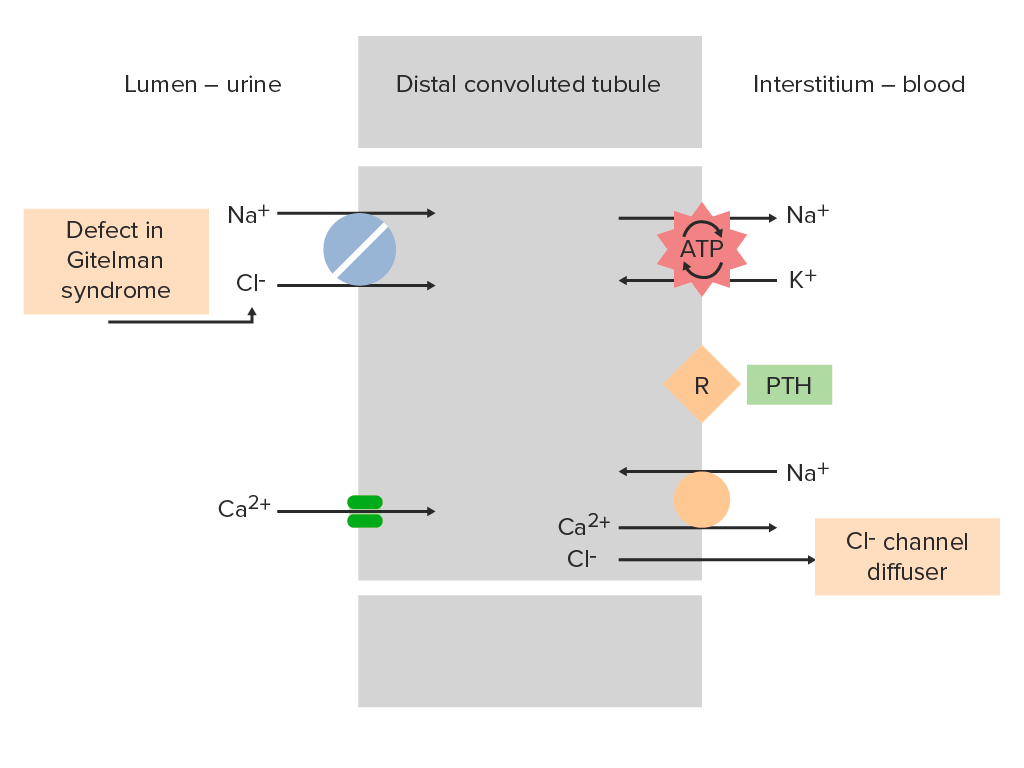
Sodium-chloride cotransporter (NCC) in the distal convoluted tubule (DCT) of a nephron:
NCC normally helps with reabsorption of Na+ and Cl- from the tubule lumen. In Gitelman syndrome, inactivation of the NCC prevents this absorption, increasing electrolyte delivery to the collecting duct. This phenomenon is similar to the mechanism of action of thiazide diuretics.
PTH: parathyroid hormone
R: parathyroid hormone receptor
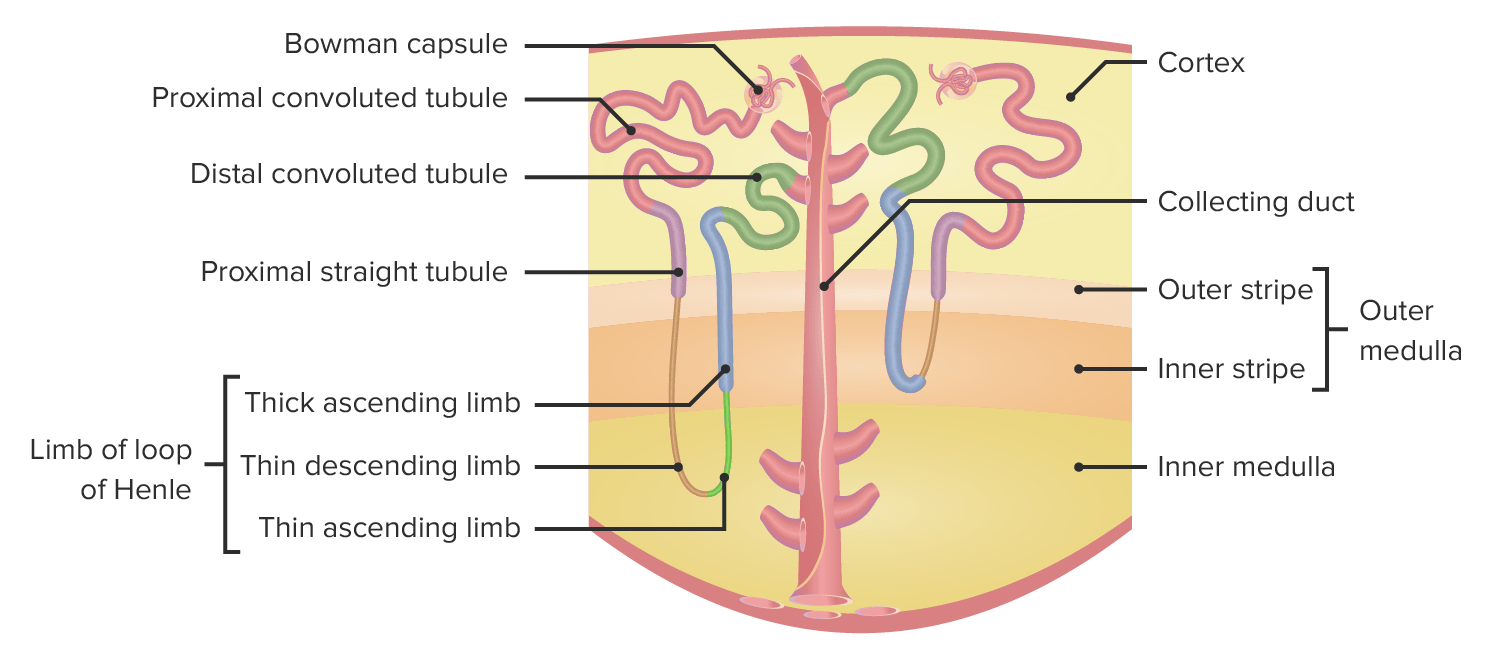
Anatomy of a nephron:
The green represents the distal convoluted tubule, which is affected in individuals with Gitelman syndrome.
Individuals with GS have mild-to-moderate symptoms without limitation in daily activity. These individuals present after the 1st decade of life in adolescence or early adulthood (rarely in infancy).
The classic clinical presentation is the triad of:
Other signs and symptoms include:
A detailed evaluation of GS is necessary when an individual presents with unexplained hypokalemia Hypokalemia Hypokalemia is defined as plasma potassium (K+) concentration < 3.5 mEq/L. Homeostatic mechanisms maintain plasma concentration between 3.5-5.2 mEq/L despite marked variation in dietary intake. Hypokalemia can be due to renal losses, GI losses, transcellular shifts, or poor dietary intake. Hypokalemia, metabolic alkalosis Alkalosis A pathological condition that removes acid or adds base to the body fluids. Respiratory Alkalosis, and normal or low blood pressure. Because of its rare occurrence compared with other renal disorders with similar symptoms, other causes should be ruled out.
Genetic testing Genetic Testing Detection of a mutation; genotype; karyotype; or specific alleles associated with genetic traits, heritable diseases, or predisposition to a disease, or that may lead to the disease in descendants. It includes prenatal genetic testing. Myotonic Dystrophies is highly specific and sensitive, and a majority of affected individuals show mutations in 2 particular genes Genes A category of nucleic acid sequences that function as units of heredity and which code for the basic instructions for the development, reproduction, and maintenance of organisms. DNA Types and Structure:
The goals of management are to minimize the effects of extracellular volume depletion Volume depletion Volume status is a balance between water and solutes, the majority of which is Na. Volume depletion refers to a loss of both water and Na, whereas dehydration refers only to a loss of water. Volume depletion can be caused by GI losses, renal losses, bleeding, poor oral Na intake, or third spacing of fluids. Volume Depletion and Dehydration and correct electrolyte deficiencies.