Pericarditis Pericarditis Pericarditis is an inflammation of the pericardium, often with fluid accumulation. It can be caused by infection (often viral), myocardial infarction, drugs, malignancies, metabolic disorders, autoimmune disorders, or trauma. Acute, subacute, and chronic forms exist. Pericarditis is an inflammation Inflammation Inflammation is a complex set of responses to infection and injury involving leukocytes as the principal cellular mediators in the body's defense against pathogenic organisms. Inflammation is also seen as a response to tissue injury in the process of wound healing. The 5 cardinal signs of inflammation are pain, heat, redness, swelling, and loss of function. Inflammation of the pericardium Pericardium A conical fibroserous sac surrounding the heart and the roots of the great vessels (aorta; venae cavae; pulmonary artery). Pericardium consists of two sacs: the outer fibrous pericardium and the inner serous pericardium. The latter consists of an outer parietal layer facing the fibrous pericardium, and an inner visceral layer (epicardium) resting next to the heart, and a pericardial cavity between these two layers. Heart: Anatomy, often with fluid accumulation. It can be caused by infection (often viral), myocardial infarction Myocardial infarction MI is ischemia and death of an area of myocardial tissue due to insufficient blood flow and oxygenation, usually from thrombus formation on a ruptured atherosclerotic plaque in the epicardial arteries. Clinical presentation is most commonly with chest pain, but women and patients with diabetes may have atypical symptoms. Myocardial Infarction, drugs, malignancies, metabolic disorders, autoimmune disorders, or trauma. Acute, subacute, and chronic forms exist. Acute pericarditis Acute pericarditis Pericarditis is usually idiopathic Idiopathic Dermatomyositis and manifests as fever Fever Fever is defined as a measured body temperature of at least 38°C (100.4°F). Fever is caused by circulating endogenous and/or exogenous pyrogens that increase levels of prostaglandin E2 in the hypothalamus. Fever is commonly associated with chills, rigors, sweating, and flushing of the skin. Fever, pleuritic chest pain Pain An unpleasant sensation induced by noxious stimuli which are detected by nerve endings of nociceptive neurons. Pain: Types and Pathways, and an audible pericardial rub by auscultation. Diffuse upwardly concave ST-segment elevations in the initial ECG ECG An electrocardiogram (ECG) is a graphic representation of the electrical activity of the heart plotted against time. Adhesive electrodes are affixed to the skin surface allowing measurement of cardiac impulses from many angles. The ECG provides 3-dimensional information about the conduction system of the heart, the myocardium, and other cardiac structures. Electrocardiogram (ECG) and pericardial effusion Pericardial effusion Fluid accumulation within the pericardium. Serous effusions are associated with pericardial diseases. Hemopericardium is associated with trauma. Lipid-containing effusion (chylopericardium) results from leakage of thoracic duct. Severe cases can lead to cardiac tamponade. Pericardial Effusion and Cardiac Tamponade on echocardiography Echocardiography Ultrasonic recording of the size, motion, and composition of the heart and surrounding tissues. The standard approach is transthoracic. Tricuspid Valve Atresia (TVA) confirm the diagnosis. Acute pericarditis Acute pericarditis Pericarditis is usually self-limiting Self-Limiting Meningitis in Children (2–6 weeks); therefore, management is conservative. If cardiac tamponade Tamponade Pericardial effusion, usually of rapid onset, exceeding ventricular filling pressures and causing collapse of the heart with a markedly reduced cardiac output. Pericarditis or constrictive pericarditis Constrictive pericarditis Inflammation of the pericardium that is characterized by the fibrous scarring and adhesion of both serous layers, the visceral pericardium and the parietal pericardium leading to the loss of pericardial cavity. The thickened pericardium severely restricts cardiac filling. Clinical signs include fatigue, muscle wasting, and weight loss. Pericarditis develops, cardiac output Cardiac output The volume of blood passing through the heart per unit of time. It is usually expressed as liters (volume) per minute so as not to be confused with stroke volume (volume per beat). Cardiac Mechanics can be severely reduced. Treatment depends on the cause, but general measures include analgesics, anti-inflammatory drugs, colchicine Colchicine A major alkaloid from colchicum autumnale l. And found also in other colchicum species. Its primary therapeutic use is in the treatment of gout. Gout Drugs, and rarely surgery.
Last updated: Dec 15, 2025
Definition
Pericarditis Pericarditis Pericarditis is an inflammation of the pericardium, often with fluid accumulation. It can be caused by infection (often viral), myocardial infarction, drugs, malignancies, metabolic disorders, autoimmune disorders, or trauma. Acute, subacute, and chronic forms exist. Pericarditis is an inflammation Inflammation Inflammation is a complex set of responses to infection and injury involving leukocytes as the principal cellular mediators in the body’s defense against pathogenic organisms. Inflammation is also seen as a response to tissue injury in the process of wound healing. The 5 cardinal signs of inflammation are pain, heat, redness, swelling, and loss of function. Inflammation of the pericardium Pericardium A conical fibroserous sac surrounding the heart and the roots of the great vessels (aorta; venae cavae; pulmonary artery). Pericardium consists of two sacs: the outer fibrous pericardium and the inner serous pericardium. The latter consists of an outer parietal layer facing the fibrous pericardium, and an inner visceral layer (epicardium) resting next to the heart, and a pericardial cavity between these two layers. Heart: Anatomy, the double-layered sac surrounding the heart.
Classification[1,3,4,6]
Clinical classification is based on duration.
| Idiopathic Idiopathic Dermatomyositis (most common) | After exclusion of other causes |
|---|---|
| Viral infection |
|
| Bacterial infection |
|
| Fungal infection (very rare) |
|
| Autoimmune disease |
|
| Metabolic |
|
| Cardiovascular |
|
| Cancer |
|
| Drugs |
|
| Features | Acute | Chronic | Constrictive |
|---|---|---|---|
| Pain Pain An unpleasant sensation induced by noxious stimuli which are detected by nerve endings of nociceptive neurons. Pain: Types and Pathways |
|
|
None |
| Other symptoms |
|
May have dyspnea Dyspnea Dyspnea is the subjective sensation of breathing discomfort. Dyspnea is a normal manifestation of heavy physical or psychological exertion, but also may be caused by underlying conditions (both pulmonary and extrapulmonary). Dyspnea |
|
| Physical examination |
|
|
|
| ECG ECG An electrocardiogram (ECG) is a graphic representation of the electrical activity of the heart plotted against time. Adhesive electrodes are affixed to the skin surface allowing measurement of cardiac impulses from many angles. The ECG provides 3-dimensional information about the conduction system of the heart, the myocardium, and other cardiac structures. Electrocardiogram (ECG) |
|
Electrical alternans Electrical alternans Consecutive QRS complexes that alternate in height. A motion artifact due to the pendular swinging of the heart within the pericardial space. Seen in large pericardial effusion or cardiac tamponade. Pericardial Effusion and Cardiac Tamponade7 with a large effusion |
|
| Echocardiography Echocardiography Ultrasonic recording of the size, motion, and composition of the heart and surrounding tissues. The standard approach is transthoracic. Tricuspid Valve Atresia (TVA)8 | Pleural effusion Pleural Effusion Pleural effusion refers to the accumulation of fluid between the layers of the parietal and visceral pleura. Common causes of this condition include infection, malignancy, autoimmune disorders, or volume overload. Clinical manifestations include chest pain, cough, and dyspnea. Pleural Effusion | Pleural effusion Pleural Effusion Pleural effusion refers to the accumulation of fluid between the layers of the parietal and visceral pleura. Common causes of this condition include infection, malignancy, autoimmune disorders, or volume overload. Clinical manifestations include chest pain, cough, and dyspnea. Pleural Effusion | Pericardial thickening |
| Tamponade Tamponade Pericardial effusion, usually of rapid onset, exceeding ventricular filling pressures and causing collapse of the heart with a markedly reduced cardiac output. Pericarditis9 | With rapid fluid accumulation | Uncommon | Never |
| Comments | Elevated cardiac biomarkers can occur, further simulating a diagnosis of acute MI MI MI is ischemia and death of an area of myocardial tissue due to insufficient blood flow and oxygenation, usually from thrombus formation on a ruptured atherosclerotic plaque in the epicardial arteries. Clinical presentation is most commonly with chest pain, but women and patients with diabetes may have atypical symptoms. Myocardial Infarction. |
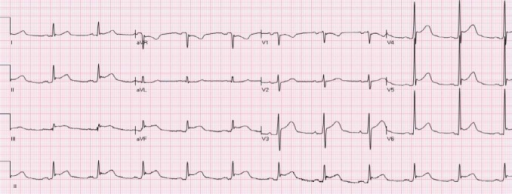
ECG in acute pericarditis, showing diffuse upsloping (upward concavity) ST-segment elevations in leads I, II, III, aVF, and V2–V6 with ST depression in leads aVR and V1 without T-wave inversions. There are also subtle PR-segment depressions in multiple leads (positive in aVR). The ST-segment elevations are caused by a ventricular current of injury associated with epicardial inflammation. The PR-segment changes are due to an atrial current of injury, also associated with epicardial inflammation.
Image: “Diffuse STE in leads I, II, III, aVF, V2-V6 with ST depression in leads aVR and V1, compatible with acute pericarditis” by Department of Medicine, Baylor College of Medicine, Houston, Texas 77030, USA. License: CC BY 3.0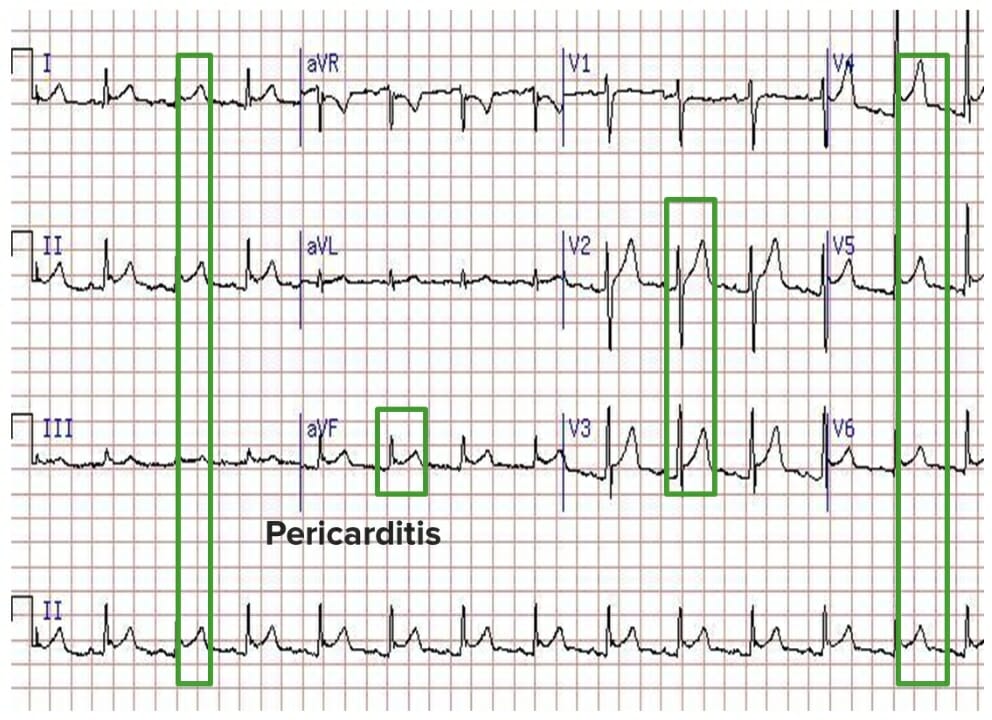
ECG showing diffuse ST segment elevation and the absence of reciprocal ST segment depression
Image by Lecturio.Based on US and European recommendations, a diagnosis can be made if the following criteria are met MET Preoperative Care:
Clinical evaluation:[1,4]
Overview in diagnostic approach:
Basic initial tests (on presentation):[4]
Additional tests:
Management can be location-specific. The following recommendations are based on US, European, and UK medical society recommendations.
Goals include:
In addition, the clinician Clinician A physician, nurse practitioner, physician assistant, or another health professional who is directly involved in patient care and has a professional relationship with patients. Clinician–Patient Relationship should look for and treat underlying etiologies.
Treatment recommendations: anti-inflammatory agents are the mainstay of management[1‒4]
Indications for hospitalization Hospitalization The confinement of a patient in a hospital. Delirium:[1, 3]
Management checklist:
Pericarditis Pericarditis Pericarditis is an inflammation of the pericardium, often with fluid accumulation. It can be caused by infection (often viral), myocardial infarction, drugs, malignancies, metabolic disorders, autoimmune disorders, or trauma. Acute, subacute, and chronic forms exist. Pericarditis occurring at least 4‒6 weeks following a first episode of acute pericarditis Acute pericarditis Pericarditis. Much less common when colchicine Colchicine A major alkaloid from colchicum autumnale l. And found also in other colchicum species. Its primary therapeutic use is in the treatment of gout. Gout Drugs is used during initial treatment. Treatment options are affected by how it presents:
Treatment:
Diagnosis Codes:
These codes are used to classify pericarditis Pericarditis Pericarditis is an inflammation of the pericardium, often with fluid accumulation. It can be caused by infection (often viral), myocardial infarction, drugs, malignancies, metabolic disorders, autoimmune disorders, or trauma. Acute, subacute, and chronic forms exist. Pericarditis, an inflammation Inflammation Inflammation is a complex set of responses to infection and injury involving leukocytes as the principal cellular mediators in the body’s defense against pathogenic organisms. Inflammation is also seen as a response to tissue injury in the process of wound healing. The 5 cardinal signs of inflammation are pain, heat, redness, swelling, and loss of function. Inflammation of the pericardium Pericardium A conical fibroserous sac surrounding the heart and the roots of the great vessels (aorta; venae cavae; pulmonary artery). Pericardium consists of two sacs: the outer fibrous pericardium and the inner serous pericardium. The latter consists of an outer parietal layer facing the fibrous pericardium, and an inner visceral layer (epicardium) resting next to the heart, and a pericardial cavity between these two layers. Heart: Anatomy (the sac surrounding the heart), distinguishing between acute, recurrent, and chronic forms of the disease.
| Domain | Code | Description |
|---|---|---|
| ICD-10-CM | I30.1 | Infective pericarditis Pericarditis Pericarditis is an inflammation of the pericardium, often with fluid accumulation. It can be caused by infection (often viral), myocardial infarction, drugs, malignancies, metabolic disorders, autoimmune disorders, or trauma. Acute, subacute, and chronic forms exist. Pericarditis |
| ICD-10-CM | I30.9 | Acute pericarditis Acute pericarditis Pericarditis, unspecified |
| ICD-10-CM | I31.0 | Chronic adhesive pericarditis Pericarditis Pericarditis is an inflammation of the pericardium, often with fluid accumulation. It can be caused by infection (often viral), myocardial infarction, drugs, malignancies, metabolic disorders, autoimmune disorders, or trauma. Acute, subacute, and chronic forms exist. Pericarditis |
| SNOMED CT | 3238004 | Pericarditis Pericarditis Pericarditis is an inflammation of the pericardium, often with fluid accumulation. It can be caused by infection (often viral), myocardial infarction, drugs, malignancies, metabolic disorders, autoimmune disorders, or trauma. Acute, subacute, and chronic forms exist. Pericarditis (disorder) |
Evaluation & Workup:
These codes are used to order key diagnostic studies for pericarditis Pericarditis Pericarditis is an inflammation of the pericardium, often with fluid accumulation. It can be caused by infection (often viral), myocardial infarction, drugs, malignancies, metabolic disorders, autoimmune disorders, or trauma. Acute, subacute, and chronic forms exist. Pericarditis, including an electrocardiogram Electrocardiogram An electrocardiogram (ECG) is a graphic representation of the electrical activity of the heart plotted against time. Adhesive electrodes are affixed to the skin surface allowing measurement of cardiac impulses from many angles. The ECG provides 3-dimensional information about the conduction system of the heart, the myocardium, and other cardiac structures. Electrocardiogram (ECG) ( ECG ECG An electrocardiogram (ECG) is a graphic representation of the electrical activity of the heart plotted against time. Adhesive electrodes are affixed to the skin surface allowing measurement of cardiac impulses from many angles. The ECG provides 3-dimensional information about the conduction system of the heart, the myocardium, and other cardiac structures. Electrocardiogram (ECG)), which often shows characteristic changes, and an echocardiogram Echocardiogram Transposition of the Great Arteries to check for pericardial effusion Pericardial effusion Fluid accumulation within the pericardium. Serous effusions are associated with pericardial diseases. Hemopericardium is associated with trauma. Lipid-containing effusion (chylopericardium) results from leakage of thoracic duct. Severe cases can lead to cardiac tamponade. Pericardial Effusion and Cardiac Tamponade.
| Domain | Code | Description |
|---|---|---|
| CPT | 93000 | Electrocardiogram Electrocardiogram An electrocardiogram (ECG) is a graphic representation of the electrical activity of the heart plotted against time. Adhesive electrodes are affixed to the skin surface allowing measurement of cardiac impulses from many angles. The ECG provides 3-dimensional information about the conduction system of the heart, the myocardium, and other cardiac structures. Electrocardiogram (ECG), routine ECG ECG An electrocardiogram (ECG) is a graphic representation of the electrical activity of the heart plotted against time. Adhesive electrodes are affixed to the skin surface allowing measurement of cardiac impulses from many angles. The ECG provides 3-dimensional information about the conduction system of the heart, the myocardium, and other cardiac structures. Electrocardiogram (ECG) with at least 12 leads; with interpretation and report |
| CPT | 93306 | Echocardiography Echocardiography Ultrasonic recording of the size, motion, and composition of the heart and surrounding tissues. The standard approach is transthoracic. Tricuspid Valve Atresia (TVA), transthoracic, real-time with image documentation Documentation Systematic organization, storage, retrieval, and dissemination of specialized information, especially of a scientific or technical nature. It often involves authenticating or validating information. Advance Directives |
Procedures/Interventions:
This CPT code is used to bill for a pericardiocentesis Pericardiocentesis Puncture and aspiration of fluid from the pericardium. Cardiac Surgery, a procedure to drain excess fluid from the pericardial sac, which is performed emergently for cardiac tamponade Tamponade Pericardial effusion, usually of rapid onset, exceeding ventricular filling pressures and causing collapse of the heart with a markedly reduced cardiac output. Pericarditis or for diagnostic fluid analysis.
| Domain | Code | Description |
|---|---|---|
| CPT | 33016 | Pericardiocentesis Pericardiocentesis Puncture and aspiration of fluid from the pericardium. Cardiac Surgery |
| CPT | 33030 | Pericardiectomy, complete or partial |
Medications:
These codes are used to prescribe the primary medical treatments for acute pericarditis Acute pericarditis Pericarditis, which include anti-inflammatory drugs like ibuprofen Ibuprofen A nonsteroidal anti-inflammatory agent with analgesic properties used in the treatment of rheumatism and arthritis. Nonsteroidal Antiinflammatory Drugs (NSAIDs) ( NSAIDs NSAIDS Primary vs Secondary Headaches) and colchicine Colchicine A major alkaloid from colchicum autumnale l. And found also in other colchicum species. Its primary therapeutic use is in the treatment of gout. Gout Drugs to reduce inflammation Inflammation Inflammation is a complex set of responses to infection and injury involving leukocytes as the principal cellular mediators in the body’s defense against pathogenic organisms. Inflammation is also seen as a response to tissue injury in the process of wound healing. The 5 cardinal signs of inflammation are pain, heat, redness, swelling, and loss of function. Inflammation and prevent recurrence.
| Domain | Code | Description |
|---|---|---|
| RxNorm | 5640 | Ibuprofen Ibuprofen A nonsteroidal anti-inflammatory agent with analgesic properties used in the treatment of rheumatism and arthritis. Nonsteroidal Antiinflammatory Drugs (NSAIDs) (ingredient) |
| RxNorm | 2683 | Colchicine Colchicine A major alkaloid from colchicum autumnale l. And found also in other colchicum species. Its primary therapeutic use is in the treatment of gout. Gout Drugs (ingredient) |
| RxNorm | 8640 | Prednisone Prednisone A synthetic anti-inflammatory glucocorticoid derived from cortisone. It is biologically inert and converted to prednisolone in the liver. Immunosuppressants (ingredient) |
| ATC | M01AE01 | Ibuprofen Ibuprofen A nonsteroidal anti-inflammatory agent with analgesic properties used in the treatment of rheumatism and arthritis. Nonsteroidal Antiinflammatory Drugs (NSAIDs) |
Complications & Supportive Procedures:
These ICD-10 codes ICD-10 Codes Pericarditis (Clinical) are used to document serious complications of pericarditis Pericarditis Pericarditis is an inflammation of the pericardium, often with fluid accumulation. It can be caused by infection (often viral), myocardial infarction, drugs, malignancies, metabolic disorders, autoimmune disorders, or trauma. Acute, subacute, and chronic forms exist. Pericarditis, such as cardiac tamponade Tamponade Pericardial effusion, usually of rapid onset, exceeding ventricular filling pressures and causing collapse of the heart with a markedly reduced cardiac output. Pericarditis (life-threatening fluid accumulation) and constrictive pericarditis Constrictive pericarditis Inflammation of the pericardium that is characterized by the fibrous scarring and adhesion of both serous layers, the visceral pericardium and the parietal pericardium leading to the loss of pericardial cavity. The thickened pericardium severely restricts cardiac filling. Clinical signs include fatigue, muscle wasting, and weight loss. Pericarditis (chronic scarring Scarring Inflammation and stiffening).
| Domain | Code | Description |
|---|---|---|
| ICD-10-CM | I31.4 | Cardiac tamponade Tamponade Pericardial effusion, usually of rapid onset, exceeding ventricular filling pressures and causing collapse of the heart with a markedly reduced cardiac output. Pericarditis |
| ICD-10-CM | I31.1 | Constrictive pericarditis Constrictive pericarditis Inflammation of the pericardium that is characterized by the fibrous scarring and adhesion of both serous layers, the visceral pericardium and the parietal pericardium leading to the loss of pericardial cavity. The thickened pericardium severely restricts cardiac filling. Clinical signs include fatigue, muscle wasting, and weight loss. Pericarditis |