Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (commonly known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Neurologic, cardiac, ocular, and joint manifestations are also common in later stages. Diagnosis relies on clinical findings and tick exposure, and is supported by serological testing. Antibiotics are used for treatment. Avoidance of tick exposure is key to prevention in endemic areas.
Last updated: Sep 4, 2025
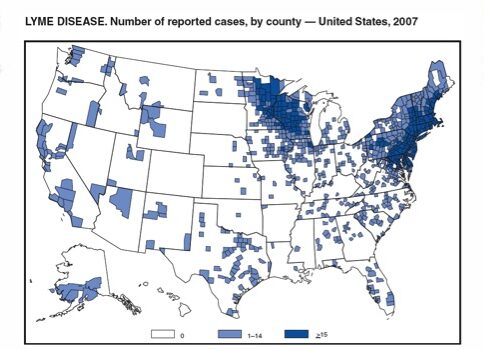
The majority of Lyme disease cases are reported in Northeastern and upper Midwestern regions in the United States, according to the Centers for Disease Control and Prevention (CDC) in 2017.
Image: “Lyme disease reported cases” by CDC. License: Public Domain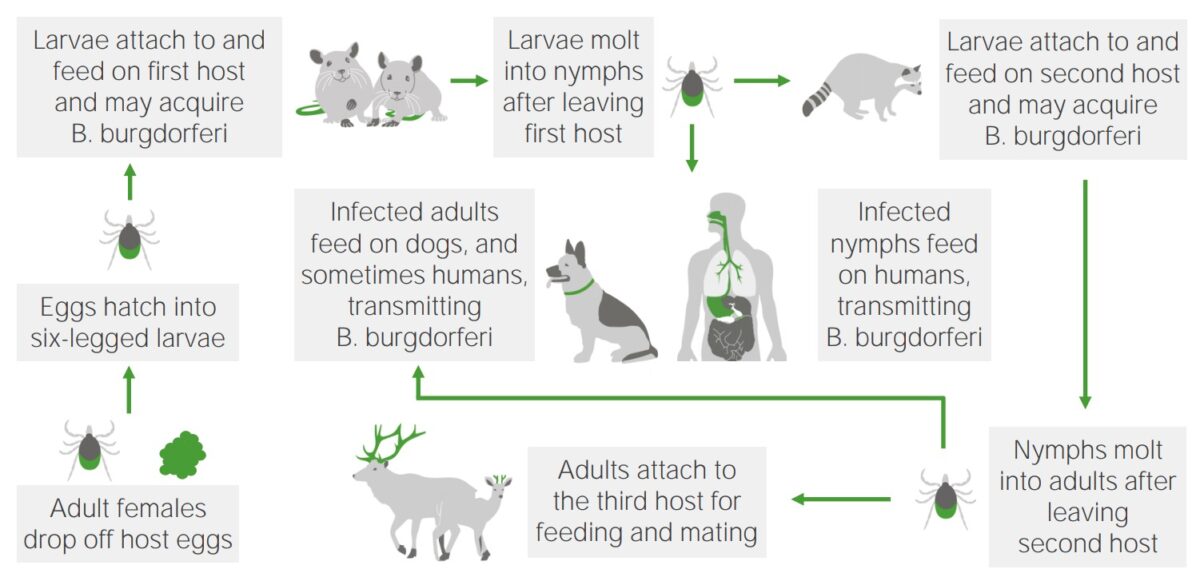
Lifecycle, reservoirs, and vector transmission of B. burgdorferi
Image by Lecturio.
The black-legged tick (Ixodes scapularis) is the primary vector for Lyme disease.
Image: “The blacklegged tick” by Liza Gross. License: CC BY 2.5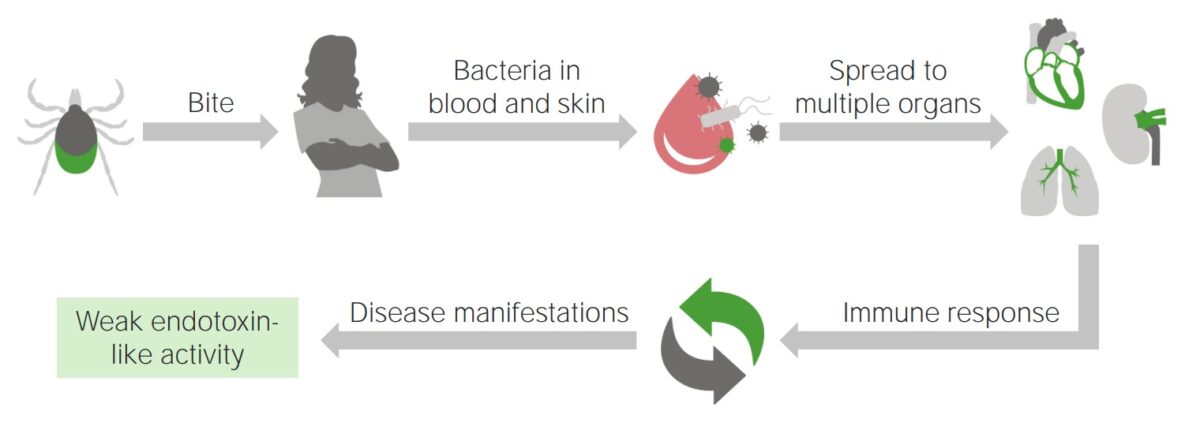
Progression of Lyme disease after a tick bite
Image by Lecturio.The incubation Incubation The amount time between exposure to an infectious agent and becoming symptomatic. Rabies Virus period for Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease is 3–30 days (mean of 7 days). The clinical manifestations of Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease are broken down into 3 stages: early localized disease, early disseminated disease, and late disease.
Symptoms appear in 1–5 weeks and resolve in approximately 30 days.
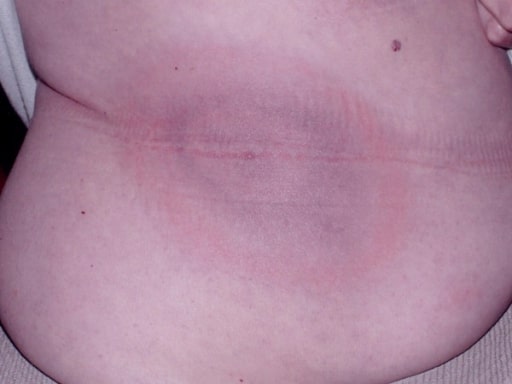
The classic “bull’s-eye” (erythema migrans) rash of Borrelia burgdorferi
Image: “Classic bull’s eye EM” by Department of Medicine, Johns Hopkins School of Medicine, Baltimore, Maryland, USA. License: CC BY 2.0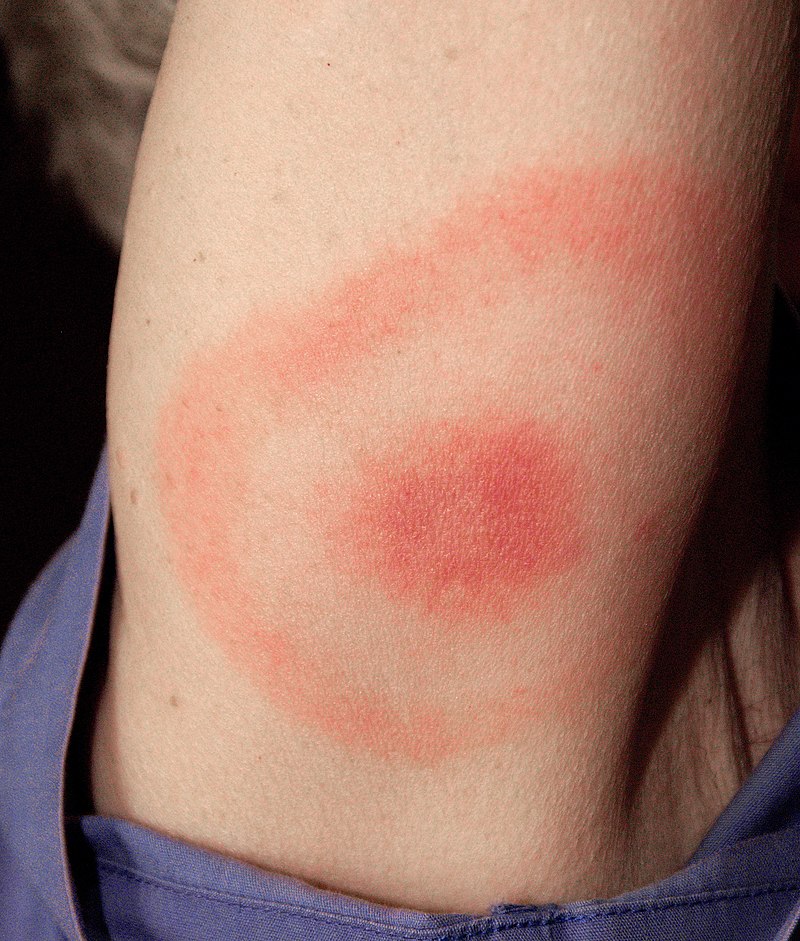
Erythema migrans
Image: “Erythema migrans – erythematous rash in Lyme disease” by James Gathany. License: CC0 1.0Symptoms develop in weeks to months in untreated patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship.
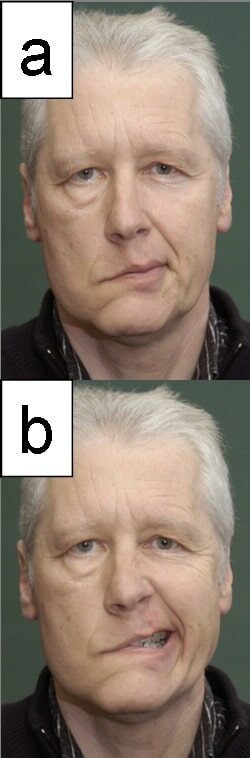
A patient with facial nerve palsy: This is the most common neurologic manifestation of Lyme disease.
Image: “Facial palsy” by Department of Otorhinolarnygology, University Jena, Lessingstrasse 2, Jena, Germany. License: CC BY 2.0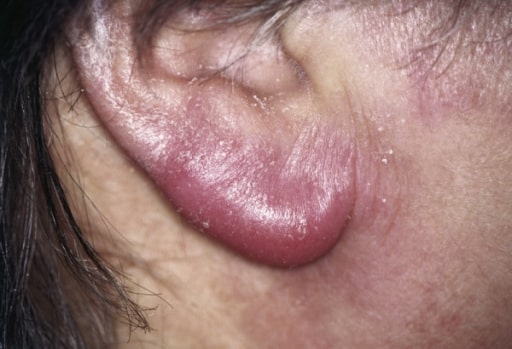
Lymphadenosis cutis benigna, also known as a lymphocytoma, of a patient’s ear: This is a rare cutaneous finding in early disseminated Lyme disease.
Image: “ Lymphocytoma” by Department of General and Visceral Surgery, Augusta Kranken Anstalt, Academic Teaching Hospital of the Ruhr-University Bochum, Germany. License: CC BY 2.0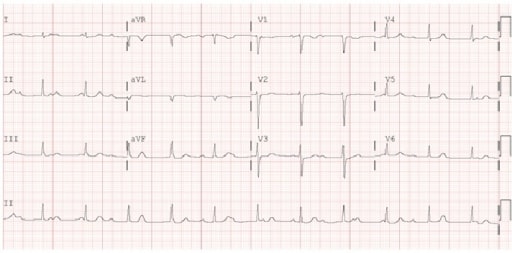
Electrocardiogram (ECG) demonstrating 3rd-degree atrioventricular block: This is 1 of the cardiac manifestations of early disseminated Lyme disease.
Image: “ Electrocardiogram” by Maxwell Eyram Afari et al. License: CC BY 4.0Symptoms develop in months to years in untreated patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship.
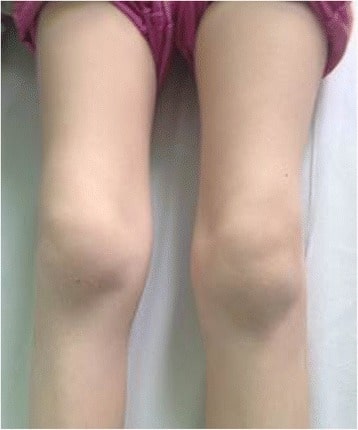
Bilateral knee swelling and arthritis in a pediatric patient with Lyme disease
Image: “Bilateral knee arthritis” by Krzysztof Orczyk et al. License: CC BY 4.0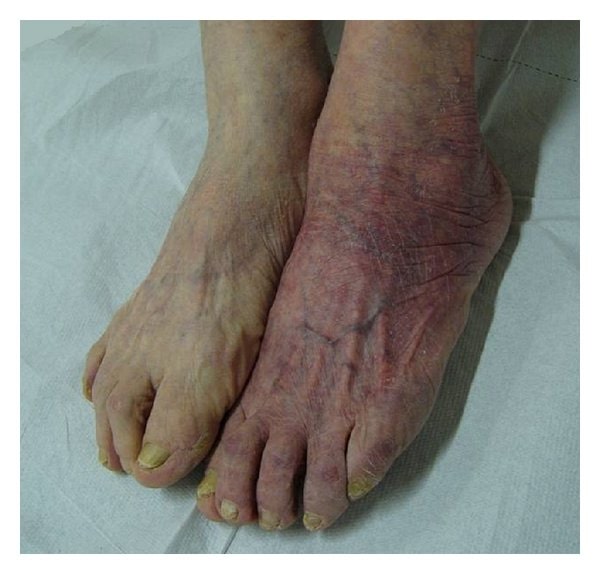
Acrodermatitis chronica atrophicans
Image: “Acrodermatitis chronica atrophicans” by Giuseppe Stinco et al. License: CC BY 3.0Common symptoms of Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease can be remembered by the mnemonic phrase “a key Lyme pie to the FACE.”
Variations in diagnostic approach can occur based on practice locations. Details of different regional recommendations (United States, United Kingdom, Europe) are available for review.
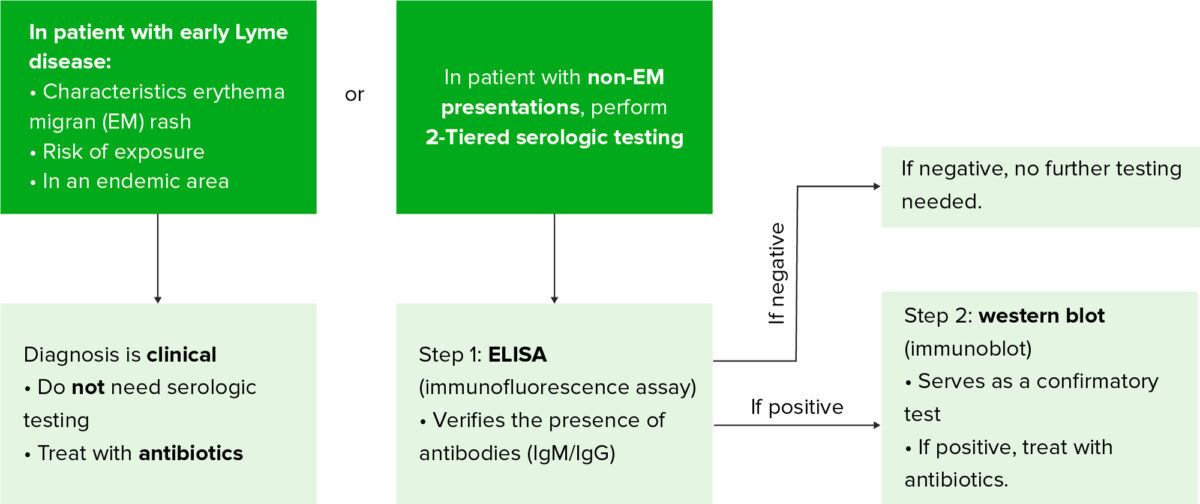
Diagnostic algorithm for Lyme disease
ELISA: enzyme-linked immunosorbent assay
Laboratory tests are only significant in conjunction with the clinical history due to a high false-positive and false-negative rate.
| Test sequence | Interpretation | Comments | ||
|---|---|---|---|---|
| Tier 1 | Tier 2 | |||
| Total IgG IgG The major immunoglobulin isotype class in normal human serum. There are several isotype subclasses of igg, for example, igg1, igg2a, and igg2b. Hypersensitivity Pneumonitis | IgM IgM A class of immunoglobulin bearing mu chains (immunoglobulin mu-chains). Igm can fix complement. The name comes from its high molecular weight and originally being called a macroglobulin. Immunoglobulins: Types and Functions immunoblot | IgG IgG The major immunoglobulin isotype class in normal human serum. There are several isotype subclasses of igg, for example, igg1, igg2a, and igg2b. Hypersensitivity Pneumonitis immunoblot | ||
| Negative | N/A | N/A | No antibodies Antibodies Immunoglobulins (Igs), also known as antibodies, are glycoprotein molecules produced by plasma cells that act in immune responses by recognizing and binding particular antigens. The various Ig classes are IgG (the most abundant), IgM, IgE, IgD, and IgA, which differ in their biologic features, structure, target specificity, and distribution. Immunoglobulins: Types and Functions to B. burgdorferi | Negative results can occur in those who have recently been infected (repeat testing recommended as indicated clinically). |
| Positive/equivocal | Negative | Negative | Antibodies Antibodies Immunoglobulins (Igs), also known as antibodies, are glycoprotein molecules produced by plasma cells that act in immune responses by recognizing and binding particular antigens. The various Ig classes are IgG (the most abundant), IgM, IgE, IgD, and IgA, which differ in their biologic features, structure, target specificity, and distribution. Immunoglobulins: Types and Functions to B. burgdorferi not confirmed | |
| Positive/equivocal | Positive | Negative | IgM-class antibodies Antibodies Immunoglobulins (Igs), also known as antibodies, are glycoprotein molecules produced by plasma cells that act in immune responses by recognizing and binding particular antigens. The various Ig classes are IgG (the most abundant), IgM, IgE, IgD, and IgA, which differ in their biologic features, structure, target specificity, and distribution. Immunoglobulins: Types and Functions detected | Consistent with
Lyme disease
Lyme disease
Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash.
Lyme Disease (acute infection); not applicable if symptoms > 30 days Retesting in 1–2 weeks can be done as indicated to check IgG IgG The major immunoglobulin isotype class in normal human serum. There are several isotype subclasses of igg, for example, igg1, igg2a, and igg2b. Hypersensitivity Pneumonitis seroconversion Seroconversion The appearance of antibodies against causative agents in the blood of individuals during the course of an infection or following immunization. HIV Infection and AIDS. |
| Positive/equivocal | Negative | Positive | IgG-class antibodies Antibodies Immunoglobulins (Igs), also known as antibodies, are glycoprotein molecules produced by plasma cells that act in immune responses by recognizing and binding particular antigens. The various Ig classes are IgG (the most abundant), IgM, IgE, IgD, and IgA, which differ in their biologic features, structure, target specificity, and distribution. Immunoglobulins: Types and Functions detected | Consistent with Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease (recent or remote past) |
| Positive/equivocal | Positive | Positive | IgM- and IgG-class antibodies Antibodies Immunoglobulins (Igs), also known as antibodies, are glycoprotein molecules produced by plasma cells that act in immune responses by recognizing and binding particular antigens. The various Ig classes are IgG (the most abundant), IgM, IgE, IgD, and IgA, which differ in their biologic features, structure, target specificity, and distribution. Immunoglobulins: Types and Functions detected | Consistent with Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease (recent or remote past); IgM IgM A class of immunoglobulin bearing mu chains (immunoglobulin mu-chains). Igm can fix complement. The name comes from its high molecular weight and originally being called a macroglobulin. Immunoglobulins: Types and Functions not applicable if symptoms > 30 days. |
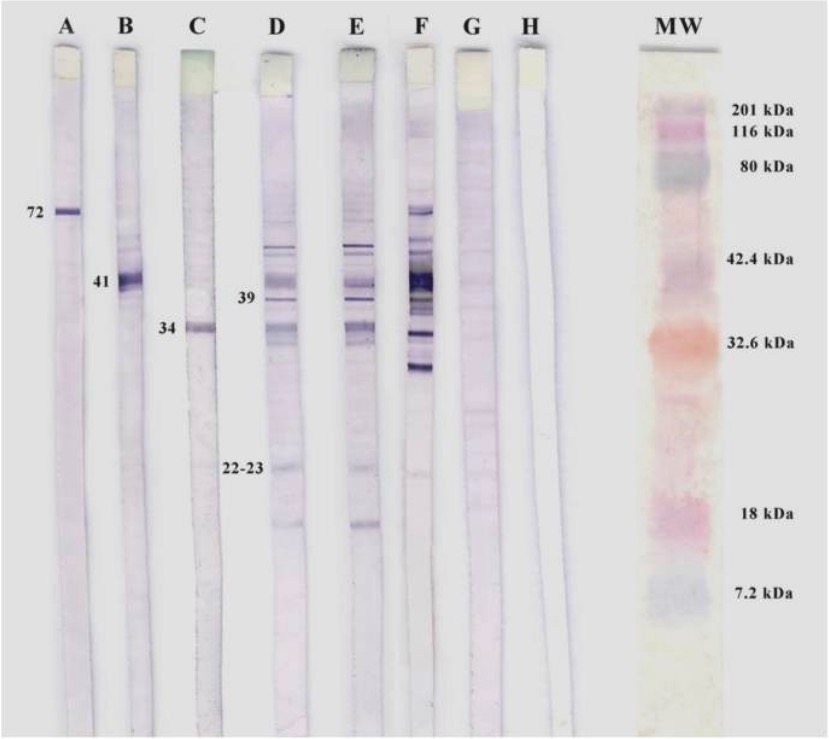
Western blotting of B. burgdorferi.
A, B, and C: positive controls for specific monoclonal antibodies
D and E: seropositive patients for IgM
F: positive control
G: negative control
H: white control
MW: molecular weight
Variations in management occur based on practice locations, and these can include (but are not limited to) antibiotic dosage Dosage Dosage Calculation and duration of treatment. The details of regional recommendations (United States, United Kingdom, Europe) are available for review.
Oral antibiotics: (used for all stages of Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease)
Intravenous (IV) antibiotics (United States):
| Clinical manifestations | Management | Comments[6,7,13,16] |
|---|---|---|
Asymptomatic patient with a tick bite requires no prophylactic treatment unless:
|
If meets criteria, then must receive prophylactic doxycycline within 72 hours of bite | Recommended dose of doxycycline:
|
| Erythema Erythema Redness of the skin produced by congestion of the capillaries. This condition may result from a variety of disease processes. Chalazion migrans (localized disease) |
|
|
| Early disseminated disease: |
|
|
|
|
|
| Cardiac and severe neurologic manifestations | Intravenous ceftriaxone Ceftriaxone A broad-spectrum cephalosporin antibiotic and cefotaxime derivative with a very long half-life and high penetrability to meninges, eyes and inner ears. Cephalosporins |
|
Late disease:
|
|
|
| Reinfection | Same antibiotic as recommended for a primary infection Primary infection Herpes Simplex Virus 1 and 2 |
Doxycycline prophylaxis Doxycycline Prophylaxis Lyme Disease is indicated if all the following criteria are met MET Preoperative Care:
Diagnosis Codes:
These codes are used to classify Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease based on its stage and manifestations, from the initial erythema Erythema Redness of the skin produced by congestion of the capillaries. This condition may result from a variety of disease processes. Chalazion migrans rash Rash Rocky Mountain Spotted Fever to later complications like Lyme arthritis Lyme Arthritis Lyme Disease or neuroborreliosis.
| Domain | Code | Description |
|---|---|---|
| ICD-10-CM | A69.20 | Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease, unspecified |
| ICD-10-CM | A69.21 | Meningitis Meningitis Meningitis is inflammation of the meninges, the protective membranes of the brain, and spinal cord. The causes of meningitis are varied, with the most common being bacterial or viral infection. The classic presentation of meningitis is a triad of fever, altered mental status, and nuchal rigidity. Meningitis due to Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease |
| ICD-10-CM | A69.23 | Arthritis Arthritis Acute or chronic inflammation of joints. Osteoarthritis due to Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease |
| ICD-10-CM | A69.22 | Other neurologic disorders in Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease |
| SNOMED CT | 21157007 | Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease (disorder) |
Evaluation & Workup:
These CPT codes are used to order the standard two-tiered serologic testing required for diagnosis: an initial ELISA ELISA An immunoassay utilizing an antibody labeled with an enzyme marker such as horseradish peroxidase. While either the enzyme or the antibody is bound to an immunosorbent substrate, they both retain their biologic activity; the change in enzyme activity as a result of the enzyme-antibody-antigen reaction is proportional to the concentration of the antigen and can be measured spectrophotometrically or with the naked eye. Many variations of the method have been developed. St. Louis Encephalitis Virus screen followed by a confirmatory Western blot test to detect antibodies Antibodies Immunoglobulins (Igs), also known as antibodies, are glycoprotein molecules produced by plasma cells that act in immune responses by recognizing and binding particular antigens. The various Ig classes are IgG (the most abundant), IgM, IgE, IgD, and IgA, which differ in their biologic features, structure, target specificity, and distribution. Immunoglobulins: Types and Functions to the Borrelia burgdorferi Borrelia burgdorferi A specific species of bacteria, part of the borrelia burgdorferi group, whose common name is lyme disease spirochete. Borrelia bacterium.
| Domain | Code | Description |
|---|---|---|
| CPT | 86618 | Antibody; Borrelia burgdorferi Borrelia burgdorferi A specific species of bacteria, part of the borrelia burgdorferi group, whose common name is lyme disease spirochete. Borrelia ( Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease) |
| CPT | 86617 | Antibody; Borrelia burgdorferi Borrelia burgdorferi A specific species of bacteria, part of the borrelia burgdorferi group, whose common name is lyme disease spirochete. Borrelia ( Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease), confirmatory test (eg, Western blot) |
| LOINC | 6335-7 | Borrelia burgdorferi Borrelia burgdorferi A specific species of bacteria, part of the borrelia burgdorferi group, whose common name is lyme disease spirochete. Borrelia Ab |
Medications:
These codes are used to prescribe the appropriate antibiotics based on the stage of Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease, including oral doxycycline for early-stage illness and intravenous ceftriaxone Ceftriaxone A broad-spectrum cephalosporin antibiotic and cefotaxime derivative with a very long half-life and high penetrability to meninges, eyes and inner ears. Cephalosporins for more severe neurologic or cardiac involvement.
| Domain | Code | Description |
|---|---|---|
| RxNorm | 3640 | doxycycline (ingredient) |
| RxNorm | 834 | amoxicillin Amoxicillin A broad-spectrum semisynthetic antibiotic similar to ampicillin except that its resistance to gastric acid permits higher serum levels with oral administration. Penicillins (ingredient) |
| RxNorm | 2240 | ceftriaxone Ceftriaxone A broad-spectrum cephalosporin antibiotic and cefotaxime derivative with a very long half-life and high penetrability to meninges, eyes and inner ears. Cephalosporins (ingredient) |
| ATC | J01AA02 | doxycycline |
These codes are used to document chronic or late-stage complications, such as Lyme carditis Carditis Rheumatic Fever ( inflammation Inflammation Inflammation is a complex set of responses to infection and injury involving leukocytes as the principal cellular mediators in the body’s defense against pathogenic organisms. Inflammation is also seen as a response to tissue injury in the process of wound healing. The 5 cardinal signs of inflammation are pain, heat, redness, swelling, and loss of function. Inflammation of the heart), or to indicate an encounter for Post-treatment Lyme Disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease Syndrome (PTLDS).
| Domain | Code | Description |
|---|---|---|
| ICD-10-CM | A69.20 + R53.82 | Post-treatment Lyme disease Lyme disease Lyme disease is a tick-borne infection caused by the gram-negative spirochete Borrelia burgdorferi. Lyme disease is transmitted by the black-legged Ixodes tick (known as a deer tick), which is only found in specific geographic regions. Patient presentation can vary depending on the stage of the disease and may include a characteristic erythema migrans rash. Lyme Disease syndrome (requires both codes) |
| ICD-10-CM | I41 | Myocarditis Myocarditis Myocarditis is an inflammatory disease of the myocardium, which may occur alone or in association with a systemic process. There are numerous etiologies of myocarditis, but all lead to inflammation and myocyte injury, most often leading to signs and symptoms of heart failure. Myocarditis in diseases classified elsewhere |
| ICD-10-CM | G63 | Polyneuropathy Polyneuropathy Polyneuropathy is any disease process affecting the function of or causing damage to multiple nerves of the peripheral nervous system. There are numerous etiologies of polyneuropathy, most of which are systemic and the most common of which is diabetic neuropathy. Polyneuropathy in diseases classified elsewhere |