Hypoparathyroidism is defined as reduced parathyroid hormone (PTH) levels due to poor function of the parathyroid glands. The cause of hypoparathyroidism is most commonly iatrogenic following neck surgery, but it can also be associated with genetic or autoimmune disorders as well as infiltrative diseases causing destruction of the normal parathyroid tissue. Deficiency of PTH results in hypocalcemia, which leads to increased neuromuscular excitability and osteosclerosis, as well as cardiac and neuropsychiatric manifestations. Treatment is based on calcium and vitamin D supplementation.
Last updated: Dec 15, 2025
Hypoparathyroidism Hypoparathyroidism Hypoparathyroidism is defined as reduced parathyroid hormone (PTH) levels due to poor function of the parathyroid glands. The cause of hypoparathyroidism is most commonly iatrogenic following neck surgery, but it can also be associated with genetic or autoimmune disorders as well as infiltrative diseases causing destruction of the normal parathyroid tissue. Hypoparathyroidism is a condition associated with insufficient secretion Secretion Coagulation Studies of parathyroid Parathyroid The parathyroid glands are 2 pairs of small endocrine glands found in close proximity to the thyroid gland. The superior parathyroid glands are lodged within the parenchyma of the upper poles of the right and left thyroid lobes; the inferior parathyroid glands are close to the inferior tips or poles of the lobes. Parathyroid Glands: Anatomy hormone (PTH). Hypocalcemia Hypocalcemia Hypocalcemia, a serum calcium < 8.5 mg/dL, can result from various conditions. The causes may include hypoparathyroidism, drugs, disorders leading to vitamin D deficiency, and more. Calcium levels are regulated and affected by different elements such as dietary intake, parathyroid hormone (PTH), vitamin D, pH, and albumin. Presentation can range from an asymptomatic (mild deficiency) to a life-threatening condition (acute, significant deficiency). Hypocalcemia and hyperphosphatemia Hyperphosphatemia A condition of abnormally high level of phosphates in the blood, usually significantly above the normal range of 0. 84-1. 58 mmol per liter of serum. Hypocalcemia are the pathognomonic biochemical features of hypoparathyroidism Hypoparathyroidism Hypoparathyroidism is defined as reduced parathyroid hormone (PTH) levels due to poor function of the parathyroid glands. The cause of hypoparathyroidism is most commonly iatrogenic following neck surgery, but it can also be associated with genetic or autoimmune disorders as well as infiltrative diseases causing destruction of the normal parathyroid tissue. Hypoparathyroidism and result directly from a lack of PTH action on the kidney.
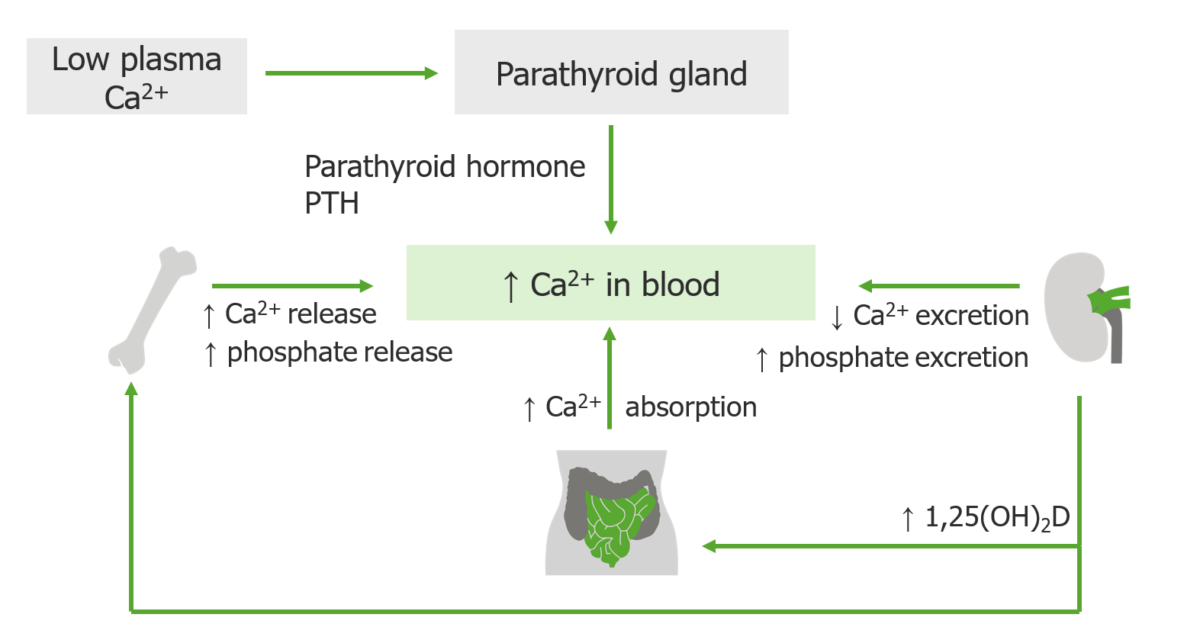
Parathyroid hormone has only one function: to correct hypocalcemia and maintain the serum level of calcium within narrow limits.
If the serum calcium is low, the four parathyroid glands secrete PTH, which is made and stored in the glands. When released, PTH works with and through vitamin D to restore the calcium level to normal.
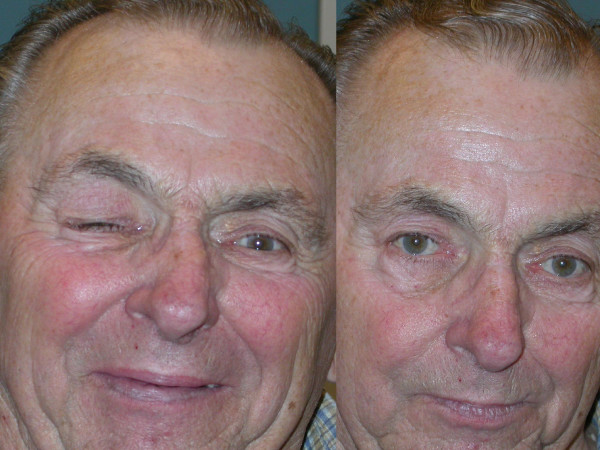
Chvostek’s sign: Induced by tapping on the facial nerve in the area of the cheek, leading to twitching of the mouth musculature
Image: “Use of botulinum toxin in head and face medicine: An interdisciplinary field” by Laskawi R. License: CC BY 2.0
Trousseau’s sign of latent tetany: Induced by applying a BP cuff and inflating to a pressure greater than the systolic pressure
Image: “Trousseau’s Sign of Latent Tetany” by Huckfinne. License: Public Domain| Diagnosis | PTH | Phosphate Phosphate Inorganic salts of phosphoric acid. Electrolytes | Vitamin D Vitamin D A vitamin that includes both cholecalciferols and ergocalciferols, which have the common effect of preventing or curing rickets in animals. It can also be viewed as a hormone since it can be formed in skin by action of ultraviolet rays upon the precursors, 7-dehydrocholesterol and ergosterol, and acts on vitamin D receptors to regulate calcium in opposition to parathyroid hormone. Fat-soluble Vitamins and their Deficiencies | Magnesium Magnesium A metallic element that has the atomic symbol mg, atomic number 12, and atomic weight 24. 31. It is important for the activity of many enzymes, especially those involved in oxidative phosphorylation. Electrolytes | Clinical clues |
|---|---|---|---|---|---|
| Hypoparathyroidism Hypoparathyroidism Hypoparathyroidism is defined as reduced parathyroid hormone (PTH) levels due to poor function of the parathyroid glands. The cause of hypoparathyroidism is most commonly iatrogenic following neck surgery, but it can also be associated with genetic or autoimmune disorders as well as infiltrative diseases causing destruction of the normal parathyroid tissue. Hypoparathyroidism | Low | High | High/low | Normal | History of neck Neck The part of a human or animal body connecting the head to the rest of the body. Peritonsillar Abscess surgery, irradiation, or autoimmune disease |
| Vitamin D deficiency Vitamin D Deficiency A nutritional condition produced by a deficiency of vitamin D in the diet, insufficient production of vitamin D in the skin, inadequate absorption of vitamin D from the diet, or abnormal conversion of vitamin D to its bioactive metabolites. It is manifested clinically as rickets in children and osteomalacia in adults. Fat-soluble Vitamins and their Deficiencies | High or normal | Low | Low (25-hydroxyvitamin D) | Normal | Bone Bone Bone is a compact type of hardened connective tissue composed of bone cells, membranes, an extracellular mineralized matrix, and central bone marrow. The 2 primary types of bone are compact and spongy. Bones: Structure and Types tenderness, weakness, and osteomalacia Osteomalacia Disorder caused by an interruption of the mineralization of organic bone matrix leading to bone softening, bone pain, and weakness. It is the adult form of rickets resulting from disruption of vitamin d; phosphorus; or calcium homeostasis. Osteomalacia and Rickets |
| Hungry bone syndrome Hungry Bone Syndrome Hypoparathyroidism | Low | Low | Low | Acute bone Bone Bone is a compact type of hardened connective tissue composed of bone cells, membranes, an extracellular mineralized matrix, and central bone marrow. The 2 primary types of bone are compact and spongy. Bones: Structure and Types uptake of Ca CA Condylomata acuminata are a clinical manifestation of genital HPV infection. Condylomata acuminata are described as raised, pearly, flesh-colored, papular, cauliflower-like lesions seen in the anogenital region that may cause itching, pain, or bleeding. Condylomata Acuminata (Genital Warts)/P and Mg after parathyroidectomy Parathyroidectomy Excision of one or more of the parathyroid glands. Hyperparathyroidism | |
| Magnesium deficiency Magnesium Deficiency A nutritional condition produced by a deficiency of magnesium in the diet, characterized by anorexia, nausea, vomiting, lethargy, and weakness. Symptoms are paresthesias, muscle cramps, irritability, decreased attention span, and mental confusion, possibly requiring months to appear. Deficiency of body magnesium can exist even when serum values are normal. In addition, magnesium deficiency may be organ-selective, since certain tissues become deficient before others. Electrolytes (impaired PTH secretion Secretion Coagulation Studies and PTH resistance PTH resistance Hypocalcemia) | Normal or low | Normal | Normal | Low |
|
| CKD CKD Chronic kidney disease (CKD) is kidney impairment that lasts for ≥ 3 months, implying that it is irreversible. Hypertension and diabetes are the most common causes; however, there are a multitude of other etiologies. In the early to moderate stages, CKD is usually asymptomatic and is primarily diagnosed by laboratory abnormalities. Chronic Kidney Disease | High | High | Low |
|
Management may vary depending on practice location and should be guided by specialist consultation (e.g., endocrinology). The following information is based on US, UK, Canadian, and European literature and guidelines for adult patients Patients Individuals participating in the health care system for the purpose of receiving therapeutic, diagnostic, or preventive procedures. Clinician–Patient Relationship.
The main indication for hospitalization Hospitalization The confinement of a patient in a hospital. Delirium relates to symptomatic or severe hypocalcemia Hypocalcemia Hypocalcemia, a serum calcium < 8.5 mg/dL, can result from various conditions. The causes may include hypoparathyroidism, drugs, disorders leading to vitamin D deficiency, and more. Calcium levels are regulated and affected by different elements such as dietary intake, parathyroid hormone (PTH), vitamin D, pH, and albumin. Presentation can range from an asymptomatic (mild deficiency) to a life-threatening condition (acute, significant deficiency). Hypocalcemia, particularly in cases of:
Monitoring and management after relevant surgery:[4,7,8,15,16,19]
Hypocalcemia Hypocalcemia Hypocalcemia, a serum calcium < 8.5 mg/dL, can result from various conditions. The causes may include hypoparathyroidism, drugs, disorders leading to vitamin D deficiency, and more. Calcium levels are regulated and affected by different elements such as dietary intake, parathyroid hormone (PTH), vitamin D, pH, and albumin. Presentation can range from an asymptomatic (mild deficiency) to a life-threatening condition (acute, significant deficiency). Hypocalcemia management:[7,10,11,13]
| Medication | Mild-to-moderate hypocalcemia Hypocalcemia Hypocalcemia, a serum calcium < 8.5 mg/dL, can result from various conditions. The causes may include hypoparathyroidism, drugs, disorders leading to vitamin D deficiency, and more. Calcium levels are regulated and affected by different elements such as dietary intake, parathyroid hormone (PTH), vitamin D, pH, and albumin. Presentation can range from an asymptomatic (mild deficiency) to a life-threatening condition (acute, significant deficiency). Hypocalcemia | Severe/symptomatic hypocalcemia Hypocalcemia Hypocalcemia, a serum calcium < 8.5 mg/dL, can result from various conditions. The causes may include hypoparathyroidism, drugs, disorders leading to vitamin D deficiency, and more. Calcium levels are regulated and affected by different elements such as dietary intake, parathyroid hormone (PTH), vitamin D, pH, and albumin. Presentation can range from an asymptomatic (mild deficiency) to a life-threatening condition (acute, significant deficiency). Hypocalcemia |
|---|---|---|
| Calcium gluconate Calcium gluconate The calcium salt of gluconic acid. The compound has a variety of uses, including its use as a calcium replenisher in hypocalcemic states. Hypocalcemia (IV) | Not applicable | 1–2 g IV bolus, followed by continuous infusion |
| Calcium carbonate Calcium carbonate Carbonic acid calcium salt. An odorless, tasteless powder or crystal that occurs in nature. It is used therapeutically as a phosphate buffer in hemodialysis patients and as a calcium supplement. Hypocalcemia (oral) | 1–3 g in divided doses (2–3 times daily) | Transition to 3–4 g in divided doses (2–3 times daily) |
| Calcitriol Calcitriol The physiologically active form of vitamin d. It is formed primarily in the kidney by enzymatic hydroxylation of 25-hydroxycholecalciferol (calcifediol). Its production is stimulated by low blood calcium levels and parathyroid hormone. Calcitriol increases intestinal absorption of calcium and phosphorus, and in concert with parathyroid hormone increases bone resorption. Parathyroid Glands: Anatomy | 0.25–0.5 µg twice daily | 0.25–1 µg twice daily |
Long-term lab monitoring and follow-up:[4,7,18]
Management:[4,6–8,11,13,15,18]
Monitoring:[4,7,8,15,18]
| Supplementation | Medication | Dose (US) | Dose (Europe) |
|---|---|---|---|
| Calcium Calcium A basic element found in nearly all tissues. It is a member of the alkaline earth family of metals with the atomic symbol ca, atomic number 20, and atomic weight 40. Calcium is the most abundant mineral in the body and combines with phosphorus to form calcium phosphate in the bones and teeth. It is essential for the normal functioning of nerves and muscles and plays a role in blood coagulation (as factor IV) and in many enzymatic processes. Electrolytes | Calcium carbonate Calcium carbonate Carbonic acid calcium salt. An odorless, tasteless powder or crystal that occurs in nature. It is used therapeutically as a phosphate buffer in hemodialysis patients and as a calcium supplement. Hypocalcemia, 40% elemental calcium Calcium A basic element found in nearly all tissues. It is a member of the alkaline earth family of metals with the atomic symbol ca, atomic number 20, and atomic weight 40. Calcium is the most abundant mineral in the body and combines with phosphorus to form calcium phosphate in the bones and teeth. It is essential for the normal functioning of nerves and muscles and plays a role in blood coagulation (as factor IV) and in many enzymatic processes. Electrolytes | 500‒3,000 mg 3 times daily | No specific dosing instructions Goal: 800–2,000 mg/day of elemental calcium Calcium A basic element found in nearly all tissues. It is a member of the alkaline earth family of metals with the atomic symbol ca, atomic number 20, and atomic weight 40. Calcium is the most abundant mineral in the body and combines with phosphorus to form calcium phosphate in the bones and teeth. It is essential for the normal functioning of nerves and muscles and plays a role in blood coagulation (as factor IV) and in many enzymatic processes. Electrolytes |
| Calcium citrate Calcium citrate A colorless crystalline or white powdery organic, tricarboxylic acid occurring in plants, especially citrus fruits, and used as a flavoring agent, as an antioxidant in foods, and as a sequestering agent. Hypocalcemia, 21% elemental calcium Calcium A basic element found in nearly all tissues. It is a member of the alkaline earth family of metals with the atomic symbol ca, atomic number 20, and atomic weight 40. Calcium is the most abundant mineral in the body and combines with phosphorus to form calcium phosphate in the bones and teeth. It is essential for the normal functioning of nerves and muscles and plays a role in blood coagulation (as factor IV) and in many enzymatic processes. Electrolytes | |||
| Vitamin D Vitamin D A vitamin that includes both cholecalciferols and ergocalciferols, which have the common effect of preventing or curing rickets in animals. It can also be viewed as a hormone since it can be formed in skin by action of ultraviolet rays upon the precursors, 7-dehydrocholesterol and ergosterol, and acts on vitamin D receptors to regulate calcium in opposition to parathyroid hormone. Fat-soluble Vitamins and their Deficiencies compounds | Calcitriol Calcitriol The physiologically active form of vitamin d. It is formed primarily in the kidney by enzymatic hydroxylation of 25-hydroxycholecalciferol (calcifediol). Its production is stimulated by low blood calcium levels and parathyroid hormone. Calcitriol increases intestinal absorption of calcium and phosphorus, and in concert with parathyroid hormone increases bone resorption. Parathyroid Glands: Anatomy | 0.25‒3 µg/day in divided doses | 0.25–2 µg twice daily |
| Alfacalcidol | Not available | 0.5–4 µg daily | |
| Cholecalciferol Cholecalciferol Derivative of 7-dehydroxycholesterol formed by ultraviolet rays breaking of the c9-c10 bond. It differs from ergocalciferol in having a single bond between C22 and C23 and lacking a methyl group at C24. Calcium Hemostasis and Bone Metabolism | 1,000‒100,000 IU daily | If used as alternative to calcitriol Calcitriol The physiologically active form of vitamin d. It is formed primarily in the kidney by enzymatic hydroxylation of 25-hydroxycholecalciferol (calcifediol). Its production is stimulated by low blood calcium levels and parathyroid hormone. Calcitriol increases intestinal absorption of calcium and phosphorus, and in concert with parathyroid hormone increases bone resorption. Parathyroid Glands: Anatomy/alfacalcidol: 25,000‒200,000 IU daily If used in conjunction to address 25-(OH)D levels: 400‒800 IU daily |
|
| Ergocalciferol | 50,000 IU weekly to daily |
Diagnosis Codes:
This code is used to diagnose
hypoparathyroidism
Hypoparathyroidism
Hypoparathyroidism is defined as reduced parathyroid hormone (PTH) levels due to poor function of the parathyroid glands. The cause of hypoparathyroidism is most commonly iatrogenic following neck surgery, but it can also be associated with genetic or autoimmune disorders as well as infiltrative diseases causing destruction of the normal parathyroid tissue.
Hypoparathyroidism, a condition of deficient
parathyroid
Parathyroid
The parathyroid glands are 2 pairs of small endocrine glands found in close proximity to the thyroid gland. The superior parathyroid glands are lodged within the parenchyma of the upper poles of the right and left thyroid lobes; the inferior parathyroid glands are close to the inferior tips or poles of the lobes.
Parathyroid Glands: Anatomy hormone (PTH), most commonly occurring as a complication of
thyroid
Thyroid
The thyroid gland is one of the largest endocrine glands in the human body. The thyroid gland is a highly vascular, brownish-red gland located in the visceral compartment of the anterior region of the neck.
Thyroid Gland: Anatomy or
neck
Neck
The part of a human or animal body connecting the head to the rest of the body.
Peritonsillar Abscess surgery.
| Coding System | Code | Description |
|---|---|---|
| ICD-10-CM | E20.9 | Hypoparathyroidism Hypoparathyroidism Hypoparathyroidism is defined as reduced parathyroid hormone (PTH) levels due to poor function of the parathyroid glands. The cause of hypoparathyroidism is most commonly iatrogenic following neck surgery, but it can also be associated with genetic or autoimmune disorders as well as infiltrative diseases causing destruction of the normal parathyroid tissue. Hypoparathyroidism, unspecified |
| ICD-10-CM | E89.2 | Postprocedural hypoparathyroidism Hypoparathyroidism Hypoparathyroidism is defined as reduced parathyroid hormone (PTH) levels due to poor function of the parathyroid glands. The cause of hypoparathyroidism is most commonly iatrogenic following neck surgery, but it can also be associated with genetic or autoimmune disorders as well as infiltrative diseases causing destruction of the normal parathyroid tissue. Hypoparathyroidism |
Evaluation & Workup:
The diagnosis is confirmed by laboratory tests showing low serum
calcium
Calcium
A basic element found in nearly all tissues. It is a member of the alkaline earth family of metals with the atomic symbol ca, atomic number 20, and atomic weight 40. Calcium is the most abundant mineral in the body and combines with phosphorus to form calcium phosphate in the bones and teeth. It is essential for the normal functioning of nerves and muscles and plays a role in blood coagulation (as factor IV) and in many enzymatic processes.
Electrolytes in the presence of a low or inappropriately normal
parathyroid
Parathyroid
The parathyroid glands are 2 pairs of small endocrine glands found in close proximity to the thyroid gland. The superior parathyroid glands are lodged within the parenchyma of the upper poles of the right and left thyroid lobes; the inferior parathyroid glands are close to the inferior tips or poles of the lobes.
Parathyroid Glands: Anatomy hormone (PTH) level.
| Coding System | Code | Description |
|---|---|---|
| CPT | 82310 | Calcium Calcium A basic element found in nearly all tissues. It is a member of the alkaline earth family of metals with the atomic symbol ca, atomic number 20, and atomic weight 40. Calcium is the most abundant mineral in the body and combines with phosphorus to form calcium phosphate in the bones and teeth. It is essential for the normal functioning of nerves and muscles and plays a role in blood coagulation (as factor IV) and in many enzymatic processes. Electrolytes; total |
| CPT | 83970 | Parathormone ( parathyroid Parathyroid The parathyroid glands are 2 pairs of small endocrine glands found in close proximity to the thyroid gland. The superior parathyroid glands are lodged within the parenchyma of the upper poles of the right and left thyroid lobes; the inferior parathyroid glands are close to the inferior tips or poles of the lobes. Parathyroid Glands: Anatomy hormone) |
Medications:
These codes are for the mainstays of treatment, which involve lifelong supplementation with
calcium
Calcium
A basic element found in nearly all tissues. It is a member of the alkaline earth family of metals with the atomic symbol ca, atomic number 20, and atomic weight 40. Calcium is the most abundant mineral in the body and combines with phosphorus to form calcium phosphate in the bones and teeth. It is essential for the normal functioning of nerves and muscles and plays a role in blood coagulation (as factor IV) and in many enzymatic processes.
Electrolytes and an activated form of
Vitamin D
Vitamin D
A vitamin that includes both cholecalciferols and ergocalciferols, which have the common effect of preventing or curing rickets in animals. It can also be viewed as a hormone since it can be formed in skin by action of ultraviolet rays upon the precursors, 7-dehydrocholesterol and ergosterol, and acts on vitamin D receptors to regulate calcium in opposition to parathyroid hormone.
Fat-soluble Vitamins and their Deficiencies,
calcitriol
Calcitriol
The physiologically active form of vitamin d. It is formed primarily in the kidney by enzymatic hydroxylation of 25-hydroxycholecalciferol (calcifediol). Its production is stimulated by low blood calcium levels and parathyroid hormone. Calcitriol increases intestinal absorption of calcium and phosphorus, and in concert with parathyroid hormone increases bone resorption.
Parathyroid Glands: Anatomy, to maintain normal blood
calcium
Calcium
A basic element found in nearly all tissues. It is a member of the alkaline earth family of metals with the atomic symbol ca, atomic number 20, and atomic weight 40. Calcium is the most abundant mineral in the body and combines with phosphorus to form calcium phosphate in the bones and teeth. It is essential for the normal functioning of nerves and muscles and plays a role in blood coagulation (as factor IV) and in many enzymatic processes.
Electrolytes levels.
| Coding System | Code | Description |
|---|---|---|
| RxNorm | 1899 | Calcium Carbonate Calcium carbonate Carbonic acid calcium salt. An odorless, tasteless powder or crystal that occurs in nature. It is used therapeutically as a phosphate buffer in hemodialysis patients and as a calcium supplement. Hypocalcemia (ingredient) |
| RxNorm | 1943 | Calcitriol Calcitriol The physiologically active form of vitamin d. It is formed primarily in the kidney by enzymatic hydroxylation of 25-hydroxycholecalciferol (calcifediol). Its production is stimulated by low blood calcium levels and parathyroid hormone. Calcitriol increases intestinal absorption of calcium and phosphorus, and in concert with parathyroid hormone increases bone resorption. Parathyroid Glands: Anatomy (ingredient) |